Blog Archives
Our London Meetup
Posted by Jennica

Dear readers, as you know, I’ve been writing about Addy’s unique face for over a decade — the feelings of being a new parent to an odd-looking child, the laser treatments with or without anesthesia, the social interactions with humor and grace, and more.
We recently had the opportunity to travel to London (from our home in the midwestern United States) and meet some of our dear blog readers IN PERSON!
These readers are, of course, fellow Port Wine Stain families, and I am SO excited to share the experience with you here.
One family traveled down from Edinburgh, Scotland with their beautiful daughter, Maia. She’s a lovely little girl whose stain, like Addy’s, covers a good portion of the right side of her face. Her port wine stain had just been treated that morning — hence the purple bruising you can see in these pictures.
Maia was a trooper! Even with cross-country travel AND a laser treatment that morning to boot, she sailed through dinner, dessert, and drinks with ongoing sweetness.
Maia charmed all of us.
In addition to Maia and her parents, we also had the immense privilege of meeting — in person! — Millie Amelia, whose own Port Wine Stain experience became its own post here. She traversed the city of London to join us after work (no small feat during rush hour!).
My own parents also joined us, as did Addy’s two siblings (our other two children, Eloise and Clarence). We all met up at a quintessentially British pub on Tottenham Court Road.
Our time together was rich. So, so rich.
It’s taken me some time to put it into words.
First, meeting in person felt like a family reunion.
It was as if we’d already known each other for years. We could feel our shared experiences without needing to figure out how to express them — experiences that are significant to us, but not common to everybody.
Maia’s parents were in good company with me and Keith as fellow parents (and even with Addy’s grandparents, too).
We’ve wondered how on earth to parent a little girl with a big blotch on her face, and keep her mentally healthy through it. We’ve pondered every angle of laser treatments, from the long-term effects of deep anesthesia to the scarring that powerful laser beams can cause on our darling daughters’ faces (which they definitely don’t need on top of their port wine stains!). And we’ve concluded that everything’s fine; these girls are fine. But it doesn’t stop us from thinking about All The Things. It’s what parents (and grandparents) do. That common ground was evident in our rich conversation.
Millie Amelia was in good company with Addy herself, as both of them are young ladies with big personalities; they also have lived the unique experience of being the only face in the room with a big blotch on it.
Millie shared with us that she’d covered her stain up with makeup for many years, and so her bare-faced confidence out in public was a relatively recent development. She and Addy have strikingly similar port wine stains — both on the right side of the face, along the V2 nerve and touching up to the forehead. Between their immediate common-ground understanding of each others’ life experiences and their similar appearance, they looked like they could have been sisters.
The pub was warm, cozy, and just crowded enough to feel festive. The food was comforting and good; we kept ordering one course after another: first some small bites… then, as we lingered, a full dinner meal… then, as we still lingered even more, a round of desserts… and then, after the grandparents had taxied back to the hotel and even the others had called it a night to get sweet Maia to bed, one more dessert as Millie and Addy continued their conversation at full speed like two sisters who haven’t seen each other in months and have SO MUCH to catch up on.
I lost count of how many times these young ladies would pause in the middle of their conversation, and stare at the other, saying, “Sorry, I just — it’s crazy — there’s someone here who looks LIKE me!”
Or, “I just can’t get over how there’s another face like mine at the table.”
Or, “It’s so weird to be with someone who looks LIKE me!”
Both of these young ladies were clearly affected by the presence of someone who looked just like them.
I hadn’t quite expected that.
At this point in the evening, only Keith and I remained at the pub with them (eating our second desserts). It was obvious to us that neither of them is terribly burdened by their port wine stains. They both enjoy looking different, and they’re accustomed to being unique. They’re used to being the odd face in the room, and they’re generally okay with that. They’re beautiful, confident, charming young women.
But that didn’t diminish the surprisingly profound impact of being in the room with someone who looks… like them. That was a new experience for both of them.
We’ve taught Addy over the years to find likeness in myriad ways. We’ve taught her to feel “like” another person with any similar trait, whether the trait is a similar hair style, same brand of shoes, matching article of clothing. We want her to feel “like” anyone and everyone, to push back any feelings of isolation that an odd-looking face might otherwise bring to her social encounters.
So it was a surprise to me that being in the presence of a face “like” hers affected Addy so profoundly. She was utterly delighted to find likeness — to find THIS likeness next to her, at the same table, looking JUST like her face.
“I can’t believe there’s someone else who looks like ME here!”
I heard many variations of that as the evening progressed, from both of these beautiful ladies.
When we finally called it a night, the pub was quiet with just a few lingering patrons, and the street was dark. Addy and Millie hugged as we departed, and we said we DEFINITELY need to do this again.
We will meet up again. After seeing the impact it had on these lovely, confident young women to be with someone else who looks “just like” them, I will be pondering new ways to meet up with new friends who also look uniquely similar.
It was, in short, a beautiful experience to meet these dear readers in person.
We thank Maia’s family for making the trip from Scotland to London (travel is never easy with a little one!). Keith and I SO enjoyed connecting with other parents in person who have thought and wondered and pondered and worried the same things we have; that’s an experience we won’t forget.
We thank Millie for making the trek across London to join us. The rest of us without port wine stains — parents, grandparents, siblings — loved connecting with this articulate young woman just a few years ahead of Addy, who could share her experiences with us.
Let’s do this again sometime.
We may live in the midwestern United States, but we’re not far from the airport, and we love to travel.
Email me at whathappenedtoherface@gmail.com to let me know where you and your port wine stain live, and we’ll gladly come celebrate it with you, too. It would be a privilege.

Posted in 3. Addy Stories & Experiences
Tags: Birthmarks, child, Coping, family, life, motherhood, Others, Parenting, Port Wine Stain
Catching Up with Teen Addy
Posted by Jennica
When Addy was born, there were a few different “future” seasons that made me nervous as a mother.
❣️I was terrified of her little heart being broken on the playground in early childhood – those moments where she would run to the swings to play with new friends, only to have bewildered stares and hold-everything “WHAT is THAT?” questions thrown at her instead.
(She survived those just fine. Kids may appear rude, but they’re just exhibiting unpolished curiosity. Once they know what “THAT” is and they’re assured she’s not in pain, the swing-pushing and new friendships carry on as normal.)
❣️I was terrified of her being THAT kid in grade school. You know the one – the easy target for the class bully, who’s usually too lazy to pick on everyone, so they fixate on that one weird-looking kid instead. I was worried she’d be THAT kid, every year, in every classroom.
(She was fine. She got a few power plays from wannabe bullies, but they were few and far between, and nothing stuck. Being unique got a LOT cooler sometime between my childhood and hers!)
❣️And I was definitely terrified of the teenage years. I saw those looming ahead when social-media culture was really taking off like a rocket. Constant comparison, airbrushed photos, self-loathing of flaws, body insecurity… it was rampant among teens, and I was deeply concerned about launching a teenage girl with an odd-looking face into that world.
Well.
Addy turned sixteen (!!) recently.
And the status of the teen years so far?
Fine.
She’s fine.
Awesome, in fact.
So, since I’m probably not the only parent looking ahead to the Teen Season with some trepidation, let me catch you up with Addy and how she’s doing, so that perhaps you, too, can breathe a sigh of relief for your own little one.
✨
First: How does she feel about her port wine stain at sixteen?
Addy LOVES her port wine stain. She wants to keep it and its current shape. Laser treatments will help it fade, and fade unevenly at that. (The vessels in the front of her port wine stain are thicker and tougher than the vessels on the side of her face, which will fade faster and cause the overall shape to change.)
So, since Addy has decided that she loves her port wine stain, we have done one – and only one – maintenance laser treatment in the last few years. I write more about Treatment #44 here; in summary, we did a clinic appointment (rather than a surgery under anesthesia), and she was awake the whole time.
The best part? The treatment successfully contained some of the growth while maintaining the shape of her port wine stain, to Addy’s liking.
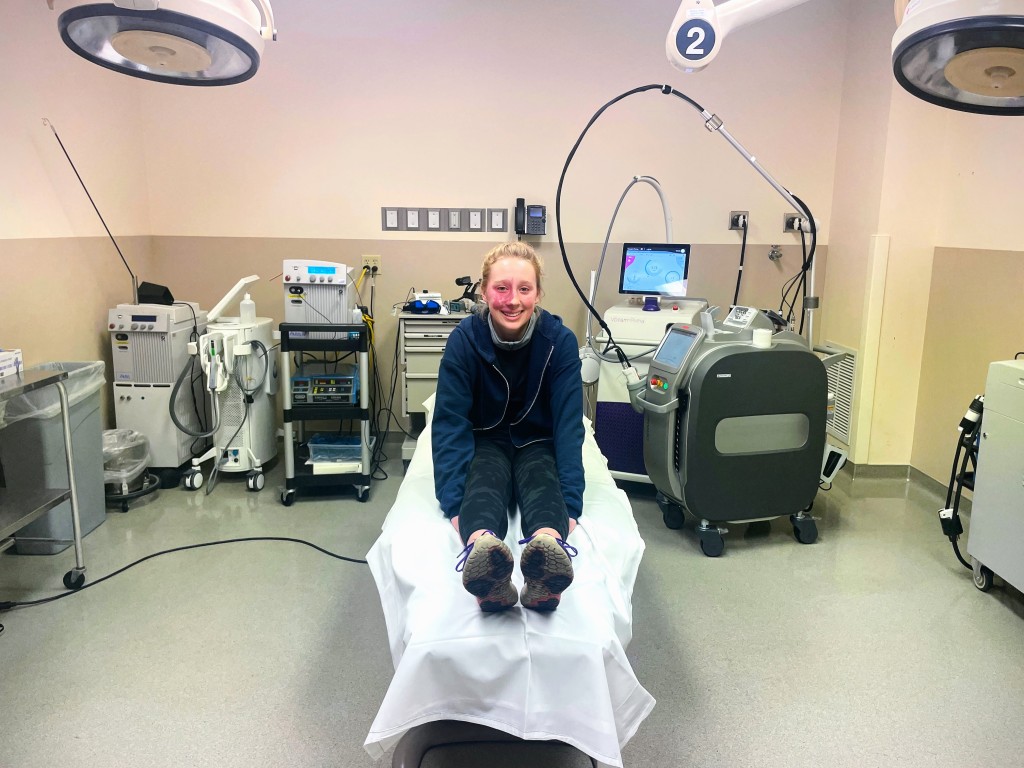
✨
What about her social life?
Addy loves humans. She loves getting questions about her face. She loves talking about it. She loves asking other people about their unique features.
She knows that imperfect people ask imperfect questions, have bad days, act crabby and mean, and can exhibit some awful behavior. She grew up with that awareness, as we prepared her to handle the myriad questions about her face with humor and grace.
In the teen years, that humor and grace have been incredible assets. She’s been training for this! Teenagers have bad days, act crabby and mean, and can exhibit some awful behavior; she lets most of it roll off her back. It takes a lot to get under her skin now.
And there has been no uptick in bad social encounters. So to those parents who are especially worried about the teen years, let me reassure you that by the time your child gets to high school, there’s a very good chance that all the other teenagers have probably already seen a lot of unique-looking humans, and your child probably won’t turn any heads or attract any undue attention for their odd face.
I say “probably” because anything can happen, but teens seem to be a lot LESS curious about the world around them than small children are, and will probably not even notice an occasional odd face. (And if you have your child in the same school from preschool through high school, as we do, then her face will be old news and already ultra-familiar to all her classmates.)
In fact, the classmates (and even the teachers and administrators!) at Addy’s school recently celebrated Addy’s birthmark on Vascular Birthmark Awareness Day, which I wrote about here.

That said, we still have some hilarious encounters, but they’re usually with younger children (like those in grade school or early middle school).
✨
Here’s an example:
One evening recently, Addy was sitting next to me in the bleachers at a high school basketball game, and we were just a few rows up from the court. Two girls walked by in front of us (they were maybe 10 years old), and when the girl closest to us saw Addy, her eyes practically bulged out of her head and her jaw dropped open.
She kept walking to keep up with her friend, but I saw her tug on her friend’s elbow, turn back, and point toward us. Apparently, her friend hadn’t seen Addy, so when there was another lull in play a couple minutes later, these same two girls walked coolly and slowly in front of us, very intentionally walking ramrod-straight, facing forward, eyes STRAINING to the side to stare at Addy as they walked by. I chuckled – I knew exactly what was going on – and pointed it out to Addy. She thought it was adorable that they were trying to get another good look at her odd face.
A few minutes later, these girls returned with a third friend, and did the same thing, ostensibly ‘showing’ their friend the sight they’d discovered. It was hilarious. These girls were clearly thinking, “WOAH!” but they were also trying SO HARD to play it cool and not stare, but they were totally staring as they did the walk-by, and it was extremely funny to watch.
Addy made sure to turn her head slightly for full visibility to satisfy their curiosity. They were delighted; they still played it cool.
So overall, the social encounters have been fewer and farther between, and as funny as ever.
✨
What about makeup?
Addy has what I’d call a healthy relationship with makeup. She uses it to enhance her features, including her port wine stain. She uses a tad bit of foundation on her face, but avoids putting it over her port wine stain, choosing instead to leave it at its full natural color. She enjoys blush but usually leaves it off, preferring to maintain a high contrast between white cheek and port-wine-stain cheek.
She’s heavy on the sunscreen, knowing that her port wine stain will be a bit more sensitive to burning and she wants to avoid injuring that skin. Smart kid.
She loves to look elegant, dressing up for school dances like a modern-day Grace Kelly.

(Had to share: For her formal last year, this lucky girl got not one but TWO parents as chaperones! Every freshman’s dream, right?)

(She had no parents chaperoning this year’s dance.)
✨
Finding Likeness

Addy still loves to find likeness in the world around her, finding her port-wine-stain pattern in everything from plants to French macarons.

✨
Addy remains the same outgoing kid who loves to interact with humans. I call her a “human golden retriever,” after the one canine breed that’s as easily social as she is.
She doesn’t worry excessively about her appearance, perhaps because her face has already been the topic of so much conversation and work over the last sixteen years, from strangers’ questions to laser surgeries and doctor’s appointments.
She doesn’t worry excessively about what other people think, perhaps because we had to train her early to let go of any concerns there, and prepare her to turn heads (for better or for worse).
She does worry about other people’s hearts, knowing that when they exhibit mean behavior, they’re probably acting out something they’ve already received themselves along the way, and she wishes better for them.

✨
The teen years were an unknown factor in the early days of our journey with Addy. Now that they’re here, I want to reassure all of my fellow parents of odd-looking children that it’s SO much better here than I anticipated.
Perhaps it’s better because we’ve already been “in training” for so many of the teenage dynamics. After all, when you’re parenting an odd-looking child, you prepare them intentionally to handle things like meanness pretty early.

Now, here in the teen years, that humor and grace are paying dividends, and it’s awesome.
This is a really fun season.
Your kiddo will be fine.
.
.
✨
P.S. I want to mention one additional note about our approach to the teen years that has helped simplify the journey for us:
Addy has no cell phone.
She is sixteen.
I will write more about that strange choice soon.
(Please know that I’m NOT judging you if you make different choices. I know many parents who need to equip their kids with communication devices for various reasons! But I will tell you that it has made the teen years MUCH easier to keep that can of worms closed entirely.)
Posted in 3. Addy Stories & Experiences
Tags: Coping, Grace, Parenting, Perspective, Port Wine Stain, School
Glaucoma-Free (so far!)
Posted by Jennica

When a port wine stain reaches up to the eye, some unique complications can result from the hypergrowth of blood vessels.
Because the blood vessels grow with the child, they continue growing ever bigger as the child grows. When the port wine stain crosses over the eye, this can lead to increasing pressure, or glaucoma. (I’ve met some port wine stain peers who have had glaucoma since childhood!)
Addy has been regularly checked for glaucoma since she was tiny, and the good news we got from her most recent ophthalmology appointment… is that she is glaucoma-free! Her eyes are working fabulously, and there is no additional pressure detected. This makes mom VERY happy. If she’s glaucoma-free now, then she’s probably in the clear. (She’ll still get checked throughout adulthood, but it’s much less of a concern as her growth slows down.)
Glaucoma hasn’t been the only concern, of course. Those big blood vessels in overdrive can cause other things, too — some of which are actually kind of funny.
In Addy’s case, when she was little, the overgrowth of blood vessels inside the port wine stain effectively close off her tear-drain-duct on the right side, causing regular overwatering of the right eye (when her normal ‘tears’ keeping her eye moist had nowhere to go). She looked like she was always crying, but only out of one eye!
To treat this, her ophthalmologist simply inserted of a drainage tube down below her right eye. They simply did this during a routine laser surgery, since Addy would already be under anesthesia. It helped to re-open the drain, and the excess tears on the right side were resolved. Easy, done.
Complications from her port wine stain will always be a concern, but as Addy gets older, our concerns shrink further. As her growth slows down, her Port Wine Stain slows down its growth, too.
(Of course, all bets are off at pregnancy, when growth goes into hyperdrive again! I know one woman who got zapped every month during her pregnancy because her Port Wine Stain started growing again like crazy.)
I expected the teen years to bring more concerns, not fewer — but as far as Addy’s face goes, it’s been nice to breathe a sigh of relief and see some of these worries settle themselves out. Her teeth (pushed to the side with all that extra blood flow and early growth on the right side) have been straightened with braces. Her right eye’s tear drain is fixed and draining normally, no longer overwatering. And her ophthalmologist says that we can pretty much not worry about glaucoma, since she’s in the clear there already.
So to all the parents out there of port-wine-stained littles, I can tell you that one by one, your worries will settle, and the menu of possible complications you might have to deal with — which seems overwhelming now — will shrink as your little one grows. There will be LESS to worry about, not more, as you reach new milestones and check these things off your list.
Your little one will be just fine.
Posted in 3. Addy Stories & Experiences
Tags: Birthmarks, Port Wine Stain, Treatments
Laser Treatment #44 for her Port Wine Stain
Posted by Jennica
Addy recently underwent her forty-fourth laser treatment for her port wine stain!
Port wine stains like Addy’s need to be treated regularly, much like weed-whacking in a garden or yard. This is because the crazy overgrowth of blood vessels that originally created the port wine stain in utero also continues to grow with the rest of the body throughout childhood.
The laser treatment, in simplest terms (because I’m a mom, not a doctor), shoots a hyper-focused beam of light at the port wine stain; that light is absorbed by the blood vessels, which heat up and die. (Their bursting is what causes crazy purple bruising after a laser treatment.)
But port wine stains vary in their depth and breadth. If the error occurred early in utero while the body was developing, then the port wine stain will be deeper and/or cover more skin; these are harder to treat. If the error occurred later, then the port wine stain will be shallower, and probably smaller in size; these are easier to treat.
The lasers can only sizzle up & kill the top layer of blood vessels. So a deep port wine stain with a lot of layers of overgrown blood vessels will be tougher to treat; they’ll appear to be “resistant” to treatment, when in fact there are just a ton of layers to zap through.
It doesn’t help that the child’s natural growth fuels further blood-vessel growth, too — and that’s why port wine stains get thicker and darker and (and perhaps bring more complications) with age.
So between the deep layers and the constant growth, Addy’s treatment schedule has looked a lot like weed-whacking in an overgrown garden. We would take a whack at the overgrowth of weeds, then wait a month, and then take another whack at the next layer.
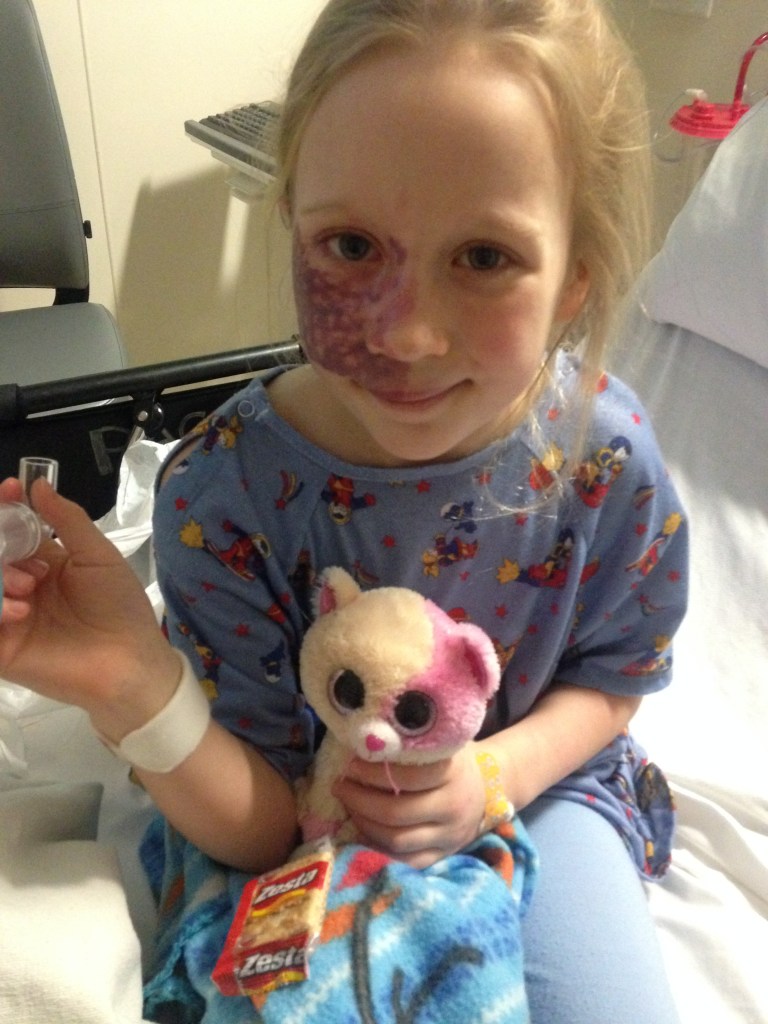
Addy’s first treatment happened when she was five weeks old, under full anesthesia. She continued to go to Children’s Hospital outpatient surgery almost every month for the first few years of her life, in order to get laser treatments for the port wine stain on her face.
Her stain was stubborn and deep! If you’re reading this and you have a baby with a port wine stain, please don’t fret — many port wine stains are NOT as deep as Addy’s, and they can go away with fewer treatments.
(And if you’re still worried that it won’t go way, you can read about Addy’s fabulous encounters with other humans here, here, and here, which only happened because her port wine stain was so visible! There are perks to being noticeable!)
Now that Addy is sixteen, she’s decided that she loves the shape and shade of her port wine stain, and wants to leave it just as is.
This means that she’ll need an occasional ‘maintenance’ treatment to contain (weed-whack!) its growth, but otherwise the treatment schedule has slowed down to maybe once a year.
This most recent laser treatment was unique: it was done in the clinic, and not in the hospital under full anesthesia.
This was new for us; her first 43 laser surgeries had all done at Children’s Hospital under full anesthesia. (This is because squirmy small children + big loud blinding laser machines pointed at their faces = sedation!)
For laser treatment #44, she saw the same dermatologist, but we went to his clinic for a quick procedure (no anesthesia).

Addy was a little bit scared going into this treatment, even at her age. She was nervous that the laser machine would be loud and would hurt her face.
She wasn’t wrong. The machine makes a loud zapping sound, which is a bit unnerving when your eyes are covered with a protective shield so you can’t see what’s coming. And the laser feels like a rubber band snapping the face a hundred times a second, so it’s not exactly painless.
But it was SO fast. She was done in about fifteen minutes. Easy.
And being a teenager, she grabbed my phone and took a selfie. Because, cool face.
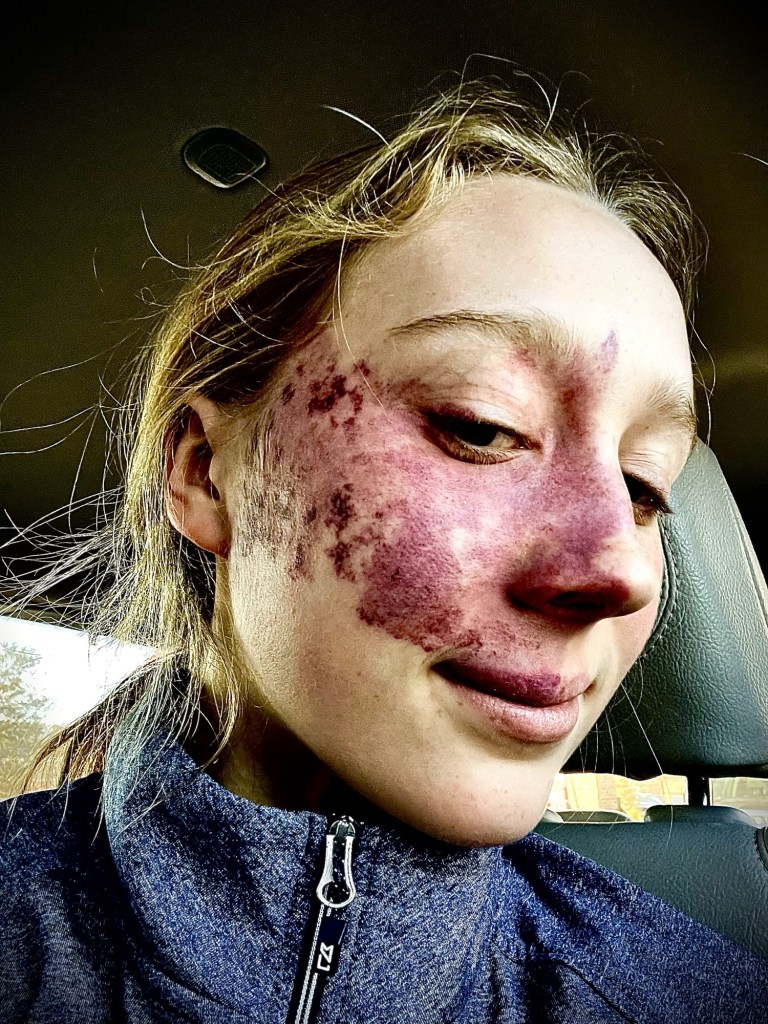
So while she definitely prefers to be knocked out cold for the procedure, she appreciated the speed with which we were done. And there was no ‘anesthesia hangover’ (which can make a person a little wobbly emotionally and otherwise for a few days afterward). And there was no need for a pre-op physical (which is necessary within the week before they’ll be going under full anesthesia). I appreciated the simplicity of it all.
There are definitely perks to both treatment approaches (under anesthesia and in-clinic). Sometimes insurance guidelines or treatment availability dictates one approach over another, and you may not have too many options.
But either way, they work, and we’re grateful for it.
If you’re looking ahead to treatment options and you want to get into this a little bit deeper, please leave a comment below and I’ll be happy to answer any questions you have!
A Few Parenting Strategies…
Posted by Jennica

How do we raise a child to love her unique face? To be self-aware, without being self-critical? Prepared for, but not scared of, encounters?
Addy’s port wine stain forced us to think through parenting moments that might have otherwise passed without notice. Getting her to a point of comfort with her face (and keeping her there) took some careful attention.
Along the way, we developed some strategies for raising a unique-looking kid. Knowing that many of you, my dear readers, are also parents and grandparents, I share 3 of them with you here.
Some of these tips might seem incredibly obvious, but they don’t always flow from us naturally.
So, bear with me if I start by stating the obvious, but here, definitely at the very most-important top of the list, is “Parenting a Unique Kid” Strategy #1:
Parenting Strategy #1: Tell her she’s pretty.
It sounds so simple.
But there is so. much. cultural noise around raising females today. And, honestly, I disagree with many of the ‘enlightened’ modern directives: “Stop telling little girls they’re pretty, or they’ll never become scientists! Just tell them they’re smart and strong instead!”
Bah, humbug. As if we’re afraid that she’ll never accomplish anything if she thinks she’s pretty. As if telling her she’s a great engineer somehow conflicts with telling her she’s pretty.
Confidence is not a zero-sum game. Building up her confidence in one area of life (brains) doesn’t take away from another (looks). So we compliment both. Profusely.
The world around my daughter will tell her, whether through magazines, billboards, TV shows, movies, fashion, petty girlfriends and rude ex-boyfriends, that she’s not pretty. Whether that’s good or bad isn’t up for debate (it’s bad). But the fact remains that there will be a hundred different ways that the world tells her she’s not pretty.
It’s my job to tell her a hundred and one (at least) that she is.
Tell your daughter she’s pretty. You’re not making her shallow, and you’re not over-emphasizing looks when you do. It’s simply an insurance policy against the jabs that this world will sling at her.
And it’s the truth anyway (right?), so speak the truth. Don’t be afraid of it. Tell her she’s pretty. And that she can run the world. Those compliments don’t conflict, no matter how much our confused culture tells you they do.
We complimented Addy’s looks all the time, from her shiny little shoes to the port wine stain splotched on her face. This girl learned early & solidly that she’s pretty. Any weird encounters over her face couldn’t even begin to burst her confidence bubble. Calling her anything less than gorgeous would be like calling Mt. Everest an anthill: simply, humorously, Incorrect-with-a-capital-I.
Yes, she also knows she’s brilliant. And funny. And creative. And empowered. We built her confidence up in all those areas by affirming them verbally, all the time.
But she needed to hear she was pretty, before the world told her she wasn’t.
So don’t worry that you’ll ruin your daughter’s brains by calling her pretty. You won’t. Tell your little engineer that she’s beautiful. She needs to hear it.
Parenting Strategy #2: Tell Her You’re Pretty
Now, take it a step further: tell your daughter that YOU are pretty.
Seriously. Look into the mirror yourself and say out loud, “I feel really lovely today.”
I know, I know – the cultural noise says we’re not supposed to. “Don’t model vanity to your child! Teach her that looks don’t matter! Focus on other qualities instead, or she’ll become a petty, vain, critical woman!”
Well, at some point, she’s going to look into a mirror. Mirrors are a part of life. And our endless human striving for self-improvement means that she will find things to improve when she does look into a mirror.
The question is, will there be any other internal self-talk running in the background that keeps that self-critical drive in check?
“I feel really pretty,” is what my daughter has heard me say for years, when doing my makeup, checking my hair, pulling on a sweater, doing anything looks-related in front of a mirror.
I started talking to my reflection like that when Addy was a baby. I realized that I would need to model a healthy relationship with the mirror; after all, this was a baby whose every glance into every mirror would be a sharp reminder that her face is not like everyone else’s around her. Every glance would show her that her face has ‘something’ different on it.
And so, I decided to vocally associate Looking in the Mirror with “Self, you’re pretty.”
Addy caught on. She began to regularly smile every time she looked into a mirror. Because as far as she knew, that’s what we women do. Her reflection smiled back.
As you can probably tell from my stories here, she is not a petty, vain, critical female, even at eleven years old. She simply knows that her reflection is lovely, and that her port wine stain is part of that reflected loveliness.
Speak out loud. Your child can’t hear your internal monologue, so say it verbally for them. And if you don’t feel pretty today, then fake it ‘til you make it, and tell your reflection that you’re pretty, because your little copycat is listening.
Can I go even further?
Brace yourself.
I also say “Cool” every time I step on a scale.
Crazy! We’re supposed to never let our daughters see us step on scales, right? We shouldn’t even own a scale, right? Otherwise, we’ll all turn into self-hating weight-obsessed confused anorexics, right?
Wrong. In my opinion, weight is a simple, factual (and sometimes even helpful) number. Facts don’t have to be scary. Checking weight is a normal part of well-child pediatric checkups, pre-op appointments, and surgeries. It’s a number. Let it be so at home. Model that.
When you step on your scale to check your weight, nonchalantly say “Cool”, no matter what the number is. Because your child doesn’t need to hear a vacuum of silence around it.
You lay the groundwork for your child’s internal monologues. These are the lines that will be playing in the back of her head every time she makes a mistake, earns an achievement, puts on a new lipstick, walks into a new lunchroom, steps on a scale, and looks in a mirror. Don’t let her inherit a vacuum of silence from you, because there are other influences ready to fill the void with commentary about how she doesn’t measure up.
Instead, equip her with confident words. Show her what it looks like, teach her what it sounds like, to be comfortable with your own self. Your own reflection. Your own body.
You won’t make her vain or shallow. It’s cool. You’re beautiful. She’s beautiful. Speak it like it’s true.
Because it is.
Parenting Strategy #3: Tell Her Others are Pretty
Are you ready? Tell her others are pretty, too.
That’s right. I provide commentary on other humans’ beauty, too.
I can already hear the chorus of enlightened shouts: “You should never comment on any other woman’s physical qualities! You’re teaching your daughter to be critical and competitive! We’re above that!”
Again: beauty is not a zero-sum game. Confidence in my own beauty doesn’t diminish my recognition of yours. Likewise, recognizing your beauty doesn’t diminish confidence in my own. It’s not an ‘either-or’ proposition, it’s a ‘both-and’.
To put it in art terms, you can admire both the clear lines of a Renaissance masterpiece and the fuzzy impressions of a Monet without diminishing either work’s value to the canon.
In human terms, you can admire the delicate lightness of an Audrey Hepburn, the glamorous strength of a Serena Williams, the stunning height of a runway model, and the voluptuous curves of an Adele – all without diminishing your perception of the others’ (or your own) beauty. Appreciating one trait doesn’t have to reduce your appreciation of a different, or opposite, trait.
But here’s the catch, parents: Appreciation doesn’t always come naturally. Visual appreciation of great art doesn’t come naturally, or children would stare at a Titian instead of a tablet for hours on end. And visual appreciation of other humans definitely doesn’t come naturally, or world affairs would look quite different. It is up to us parents to endow our children with a deep appreciation of that which is truly beautiful in the world, including other humans.
Too often, we’re told never to comment on anyone else’s looks, because that should be left to our shallow, self-obsessed, critical, vain, popular culture, and we should be above that.
But if that’s the only commentary your child hears (and until a nuclear apocalypse wipes out said pop culture, your child will hear it), then you’ve left a vacuum of silence where there should be positive appreciation.
So compliment the beauty in others. Freely tell your daughter what you find beautiful. I’ve complimented many different birthmarks, skin tones, heights, ages, and weights to Addy. Thus, she has learned that there is beauty in those various birthmarks, skin tones, heights, ages, and weights (including, naturally, hers, wherever she may be in life).
Your commentary allows your daughter to begin spotting beauty in other humans to a greater degree of diversity than she might otherwise pick up on her own. You just have to help her spot it in the first place. This is critical. Don’t let her get silence from you on this.
Because later, she will be tempted to feel down on herself for not ‘looking like’ the Beautiful People… a feeling that usually rests on a pretty narrow view of beauty. The more variety she sees as beautiful now, the harder it will be to peg down exactly what requirement she’s not meeting later.
Point out the beauty in all the other humans; compliment a full spectrum of diverse features, so she learns to appreciate them all. Then she’ll learn to appreciate hers, too.

Posted in 3. Addy Stories & Experiences
Comments Off on A Few Parenting Strategies…
Tags: Birthmarks, Coping, Parenting, Perspective, Port Wine Stain
You’ll Be Okay
Posted by Jennica
Congratulations! You have welcomed a new baby into this world. You are excited, happy, terrified, uncertain.
And that baby looks nothing like what you expected.
If you, too, have been surprised by your perfect newborn’s unexpected face, I can perhaps offer some insight into the things you’re worrying and wondering about.
You already knew that you’d have to navigate the challenges of raising a child in this complicated modern world, but you weren’t prepared to do it with a strange-looking face.
You may be torn between calling your perfect little infant “perfect” and wondering what to do about this looming flaw. Should you call it a flaw? Will she think she’s not perfect? Should you mention it to her at all?
You will Google this condition, and when you see all the ways these errant blood vessels can invade the brain, the eyes, the nose, and the gums, you will start watching for every daily milestone to make sure all systems are working the way they should. At least, for now; those vessels will keep growing.
You will feel guilt at your concern over your baby’s face while other parents are dealing with issues so much more deep, painful, and immediate than this ‘cosmetic’ issue; yet, when someone else tells you to be thankful that you have “only a cosmetic issue” to deal with (and maybe even that “it’ll go away”), you’ll want to cry.
You will worry over every contact sport, every scratch, and every nosebleed, along with her eyes, gums, tongue, teeth, brain, and anything else these overgrown blood vessels touch.
And then, you will wonder what you’ll eventually say to her. How will you talk to her about it? And it will feel a lot like vanity, worrying about her looks, and surely, you’ve never been this vain before…
When it comes to her looks, you will struggle in the balance between truths – the truths that other people tell you, and the truths you discover for yourself.
People will tell you your baby is beautiful, and that’s true. They will tell you that your child will be absolutely fine sporting a birthmark in our enlightened modern era, and that’s true. They will tell you that beauty is so much deeper than skin, and that’s true. They will even tell you that people hardly notice it after they meet your child, and that’s true, too.
But it’s also true that the uniqueness of each birthmark means that your child may never see another human being like them, and that’s isolating. It’s also true that your decision to treat, eliminate, remove, or otherwise ‘fix’ this error will haunt your parenting conscience whether you choose to leave it or not, and that’s sobering. It’s also true that our human instinct to spot aberrations in nature means that your child’s errant face will never not be spotted, and that’s overwhelming.
It’s a worrisome thing to raise a child with a strange face. It’s okay that you’re dealing with those worries; it doesn’t make you a shallow person. And you may not feel validated when people encourage you with all the truths about how cool it is to have a birthmark now; they’re not wrong; it just doesn’t feel validating. That’s okay, too. Take their encouragement; consume the truth they’re giving you.
You will think ahead to the first day of preschool, and the first day of kindergarten, and all the other firsts that she will walk into. How will she carry herself into the room? What will she say?
You will find yourself noticing all the unique features in other humans now. And every time you see another human with a Thing on their Face, you’ll devour every hint that might give you clues to your own daughter’s future, all the way down to the way that one birthmarked guy orders his ice cream, and the way that one birthmarked girl slouches into her hoodie. Ashamed? Is that what your perfect, brilliant, precocious infant daughter will become?
People can assuage you all they want, but let me tell you, when you think ahead to all the things you have to prepare a daughter for these days, and then plan on having a weird face on top of it, it’s overwhelming.
You may not know what to do with all the overwhelmingness. You may be quick to feel indignance: How dare Disney not have a princess that looks like my daughter? You may be quick to feel offense: How dare that ignorant idiot ask my daughter what’s on her face?
Take a deep breath; be patient with all the other flawed humans around you. They may not validate your concerns; they may not accommodate your daughter’s face, or even anticipate it. They may ask loud questions. That’s okay.
Have grace for other humans; give them room to err, because they’re imperfect, too.
Have a sense of humor; dress your baby up as a Dalmatian puppy on Halloween and call her ‘Spot’, because you only live once.
We’re reluctant to embrace vanity, but when we’re honest, we would admit that we desperately want to conform, we want to look “like”, and we want to be seen as pretty. This is our vanity, and we feel guilty for it, and a facial mark rocks that guilt. It may feel better to preemptively blame other humans for not accommodating your daughter in their princess lineup, but I think it’s healthier to admit that a natural dose of vanity comes with being human. It doesn’t make you a bad person.
It’s okay to worry about all of this, and then it’s okay to let it all go and take “Spot” trick-or-treating.
Parenting is always uncharted territory. Every child is unique, and every day is new. I can give you advice, I can tell you what we’ve learned; but, ultimately, you will make your own path. I’ve walked some of your steps, but not all of them.
And as I learn from each of our steps, I will continue sharing what we’ve learned with you, here. But in the meantime, please know that I’ve felt what you’re feeling, and I can tell you, after more than a decade of parenting a Kid with a Thing on her Face, that it’s all okay.
Addy may not remember being dressed up as a Dalmatian puppy named ‘Spot’, but she thinks the pictures are hilarious. She’s fine. It’s all good.
You’ll be fine, too.
P.S.: I wrote a few “Parenting Strategies” posts you may enjoy. Here is the first in that series.
Posted in 3. Addy Stories & Experiences
Tags: Birthmarks, Coping, Encounters, Grace, Parenting, Perspective, Port Wine Stain
Medical Comfort
Posted by Jennica
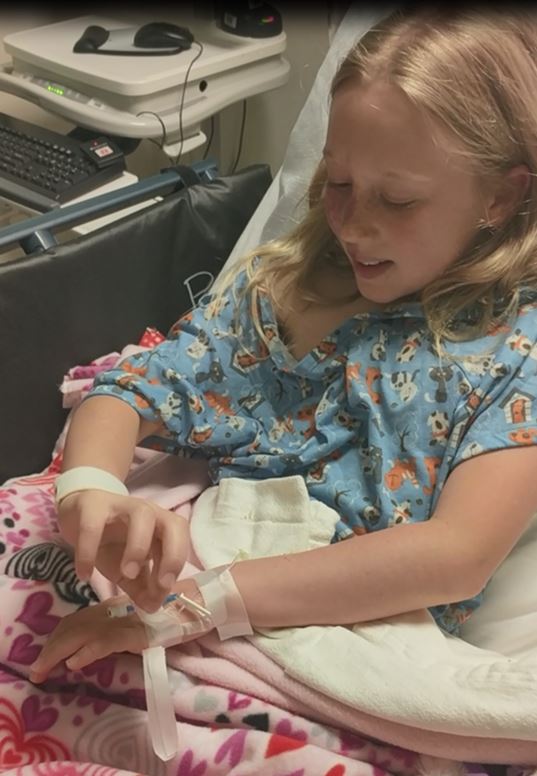
For Addy’s first few years of life, she lived by a cycle of monthly laser surgeries: she was at Children’s Hospital for a new surgery every month; three weeks later, she’d go to the clinic for a pre-op checkup, then go back to the hospital for another surgery the following week. Three weeks later, another pre-op, then another surgery; then another pre-op, and another surgery… you get the cycle.
The surgeries are minor, thank goodness, but many. She’s had 43 laser treatments (so far) under anesthesia beginning at 5 weeks of age, each one variously bringing IVs, yucky-tasting drugs, and masks covering her face, and each one preceded by a pre-op appointment with a clinic doctor the week before.
Every medical encounter, with all its variables, carried the risk that Something might happen to turn her off from medical appointments. Shots, exams, drugs, questions, strange surroundings, weird lights, being transported in a moving bed – all of these things can be painful or disorienting, and the likelihood that Addy might end up hating all things medical was always high.
Yet you’ve probably noticed (here, here, and here) that for Adelaide and her Port Wine Stain, medical settings are happy places.
So how did she arrive at her love of all things medical? Why is she so comfortable as a patient? I hope that for any parent reading this who has a child requiring a minor (if frequent) medical procedure, our insights here might help smooth the experience.
It comes down, broadly, to two things:
1) medical providers who understand children, and
2) some very intentional parenting at every single appointment.
First, those providers:
Seek out children’s medicine if at all possible. All of Addy’s surgeries have taken place at a Children’s Hospital, where every single worker is oriented to children, not just as smaller versions of adults (which they’re not), but as their own species. Their bodies are different. Their brains are different. One can’t always explain things to a kid, one usually can’t reason with a kid, and one forgets what frightens a kid’s brain, but at Children’s, all these things are on the radar of every nurse, receptionist, doctor, assistant, and specialist. That’s not to say that they’re all perfect all the time, but it’s a great place to start.
Outside of Children’s Hospital, our other providers ‘get’ kids, too. Her primary care doctor is a pediatrician. Her dermatologist, while not a pediatrician, is a laser expert who specifically treats children with port wine stains. Her ophthalmologist is a pediatric ophthalmologist (glaucoma is one of the possible complications from a port wine stain), and I can’t imagine trying to do that long, strange appointment with anyone other than a children’s eye doctor.
At these appointments, we’re just as likely to be asked about favorite cartoons as we are about recent colds. The pediatrician doesn’t just look in her ears at a checkup, he ‘looks for’ Disney princesses or Marvel characters. The ophthalmologist speaks more to Addy during her eye check than to me, and that’s perfectly fine.
With so many opportunities for bad experiences, taking your child to a provider that understands children is a great place to start.
The second major factor: the parenting.
If you want (or need) your child to be comfortable in medical settings, then you need to intentionally parent through every medical encounter, even the small ones. You’ve seen some of my specific tips before, but this provides some wider context.
Always, always, remember this: You are the parent. You run the show. Therefore, when you take your child into any medical setting, here are 5 things I want you to keep in mind:
- Choose your attitude wisely, for your child will absorb it and then reflect it. Be positive.
When you visit a Children’s hospital a lot, you pick up on certain patterns, like this one: no matter the personality of the child, they’ll always end up reflecting their parents in the waiting room.
Pre-procedure parents are either Relaxed & Happy, or they’re Nervous About What’s Coming (complete with pursed lips and bulging neck veins). They’re either smiling with their child, or tensing up like a guitar string about to snap.
Can you guess what happens to the child in those few minutes in the waiting area?
Within moments, they absorb the signals emanating from their parent, and then they unconsciously match them. Happy parents? Happy kid keeps playing. Tense parents? Kid does a double-take at the awesome toys in front of him, decides that maybe there’s something sinister about them, gets really quiet, goes over to Mom & Dad, and sits quietly, whining occasionally.
When it comes to your child in medical settings, remember that YOU set the tone. You are the sky, and your child is the lake. If you’re sunny and bright, then the water shines brightly, too; if you’re cloud-covered and gloomy, then the water is grey and cloudy, too.
You carry immense responsibility. Your child will reflect you. If you want them to come out of a clinic appointment happy, then you can’t walk in like you’re about to get that awful shot you got back in 1998. If you want this surgery to not be a negative experience, then you can’t walk into the hospital looking like you’re on your way to a funeral. If you want your child to comfortable in medical settings, then you must first be comfortable here.
And if you have to fake it ‘til you make it, then fake it, because your little copycat is taking their cue to be either happy or terrified from you. Don’t lie about anything (more on that below); just make sure that their starting point isn’t “terror”.
- Remember your child’s natural ignorance.
Look around the hospital or examination room at all the strange objects from a kid’s perspective: you may be familiar with the blood pressure cuff, but your child is not. For all he knows, it’s a torture device. Preempt his fears by telling him what everything is. Explain, explain, explain, and always with a positive attitude. Good nurses and assistants are great at this; when one of them takes Addy’s blood pressure, they first hold the cuff up and say, “Do you know what this does?” with big smile and an air of intrigue, piquing the child’s curiosity. “It’s going to give your arm a tight hug.”
There. Done. The strange object has been acknowledged and explained, just enough to reassure the child that it won’t be used for anything sinister. Can you imagine trying to get a blood pressure reading without doing that first? The poor kid has this thing strapped on his arm, there’s a buzzing sound, and then all of a sudden it cinches tighter and tighter and tighter and he’s wondering, “Where are we going with this? Give me back my arm!”
Now, this ignorance comes with a bonus: Kids aren’t born knowing that medical stuff is bad. That’s the burden we adults carry because we’ve visited hospitals when loved ones are at death’s door, when accidents change our lives forever, when babies are born dangerously early. We understand life and death, and we know that the treatment can hurt more than the disease; if we had to check ourselves in today, we’d probably freak out. So we expect the same trepidation from our children.
But to your child, all of this is new. And a child is accustomed to encountering new things every day; that’s part of being a young human. They’re constantly facing unfamiliar people and experiences and objects, whether at the grocery store or the hospital. There’s no need for any of it to be negative at the start, so don’t heap that upon them. They’re starting fresh.
Marvel at the blood pressure cuff with them – isn’t that cool how it works? Handle the mask together and laugh about how it looks on your face. Explain what these things do. Mysterious unknown objects can be scary; familiar everyday objects aren’t. Get a ‘play doctor’ kit with a stethoscope and blood-pressure cuff. Ask the hospital if you can take home a mask so you can play ‘surgery’ at home and have a blast. Let them be curious, help them explore, and keep everything positive.
- No surprises. Ever.
Some people want to distract a child so they don’t see a shot coming, and then they sneak it in, thinking that it makes the overall experience shorter and easier. Trust me, that only works once. The child cannot logically process, “Well, gee, that was SO much more efficient.” All they know is, “OWW!! What?!?!”, and they will never, ever, ever again trust that stranger in the white coat, or even you in that environment. Which means that the next time you carry them into a clinic or hospital, they’ll be inconsolable.
When I was a child, I was a patient in a hospital that wasn’t a children’s hospital. No one there knew how to handle kids, and they administered shots by the ‘distract & surprise’ method. It didn’t take long for me to distrust every white-coated person I encountered thereafter; I even freaked out if I saw a white winter jacket outside the hospital.
Do not let anyone (nurse, tech, or doctor) surprise your child with something unpleasant. Take an extra moment ahead of time to warn your child what’s coming. Note the word, ‘moment’ – no need to linger on the idea, just a few extra seconds to clearly, openly, and (most important) matter-of-factly tell your child what’s coming. (Remember, if you freak out, they’ll freak out.)
Keith was the master of this disclosure. Knowing we had a long medical road ahead of us, he left nothing to chance, even seasonal flu shots and routine blood draws. Whenever a procedure came, here’s how it would go down:
The tech would prepare the shot.
Keith would turn to little Addy and say:
- “Sweetie, you’re going to get a shot now.” [tell ‘em what’s coming]
- “It might hurt, and that’s okay.” [matter-of-fact warning, NEVER negative]
- “We’ll count to three,” [a consistent system she can rely on each time]
- “…she’ll poke you once, and then we’ll be all done.” [finite ending – the light at the end of the tunnel]
He’d nod to the tech; they’d gently anchor her and count to three together, and the tech would poke Addy on “three.” Addy might cry for a moment, but Keith would immediately scoop her up and affirm her: “There, see? All done! All done, just like we told you.” [Remind her that it went down exactly as you said; she can trust you.]
“Now, tell the nice lady ‘thank you’.”
That’s right, he made her politely thank every tech and nurse who took care of her, even those who administered shots. An attitude of thanks may sound crazy, but for a little toddler, the effort of articulating polite words of gratitude provided enough of a distraction (after all, that’s a lot of work when you’re two) to get her mind off any lingering pain from the quick shot. And it fended off any possible “poor me” wallowing that could creep in among her many medical visits, to acknowledge the role of all caregivers around her, even those stuck doing thankless tasks.
Sniff, sniff, “Tay too [thank you].”
And with that, the event is done. Your child knows that you’re trustworthy, consistent, and dependable. We haven’t been allowed to wallow. The pain is disappearing. What were we crying about again? Now, go get a sticker, and the day is made. (If we’ve gone under anesthesia, then go get a popsicle, and the whole WEEK is made.)
No surprises. Medical procedures don’t have to be pleasant, but they definitely should not be a surprise. Ever.
- Be your child’s activist when it comes to details of treatment.
Even in these great settings, we occasionally encountered providers who weren’t perfect. One clinic nurse was so nervous around kids that she clumsily administered a “surprise” shot to the leg really hard, without giving Keith a chance to count Addy to three. Bad idea. Addy felt shocked & betrayed, it took Keith over an hour to calm her down, and the poor kid limped for a week. Not a good thing when we were bringing her in for a medical appointment or procedure every 1-3 weeks.
Needless to say, we were more demanding of procedure thereafter. We had a lot grace for the nice nurse’s nervousness (after all, no sweet soul actually wants to administer shots to children), but we did discreetly discuss the event with the clinic, and they were awesome. They understood that we couldn’t afford to have Addy not trust us, and they helped ensure that all shots thereafter followed a trustworthy procedure.
Remember, again, you’re in control. Your child takes their cue from you, and the providers take their cue from you; if you’re not comfortable with some aspect of treatment, they’ll probably work with you until there’s some resolution. But they can’t read your mind, so speak up. Be kind and courteous, and they’ll work with you.
- Empower your child to do things themselves
I was surprised one morning when a nurse at Children’s Hospital offered to let Addy take out her own IV after a surgery. Taking out the IV has always been a nasty moment, mostly because of the adhesive sticking to the skin. (The needle is nothing compared to that sticky hand-hair-grabbing tape!) Addy was always apprehensive about getting the IV out.
But then the nurse showed Addy how to pull it out herself, and it turned that moment from one of apprehension to one of empowerment. Addy learned exactly how the IV worked, where the line was, and how fast to pull off the tape. Altogether, it made her feel awesome. No more tears.
Expect great things of a kid, and they’ll rise to the occasion. I’m grateful for that nurse’s wisdom; she knew Addy could handle the task herself, even if I didn’t.
Keep your eyes open for opportunities to let your child do things for themselves in medical settings; ask the provider if a task can be done or assisted by the patient herself. The IV task has been rather empowering for Addy, and there might be others. The providers can help you find ways to empower your child to do things themselves, especially if they’re used to working with children.
Yes, perhaps you’d rather be at a tropical beach than at yet another procedure, but honestly, it could be worse, and in the grand scheme, it’s really not so bad. So enjoy the little stuff; get excited about stickers and pumped about popsicles, because then your kid will, too. Savor the time with your child (and a good book during those precious quiet minutes when they’re under anesthesia). Life is beautiful, this laser treatment stuff isn’t so bad, there’s a whole team of people taking care of your offspring. And with luck, your offspring will realize that it’s all quite lovely, too.
**Post script: I will never forget the evening we went out to dinner to celebrate Addy’s 5th birthday. By chance, we ended up seated in a booth just behind Dr. Steelman, the pediatrician who has seen her through all of her medical ‘stuff’ since she was a newborn – and therefore a provider she could either love or loathe. When Addy caught a glimpse of him out of the usual medical context, her face lit up like a Christmas tree and she stammered excitedly, “Uncle Steelman!”
Priceless.
Going in for a Laser Treatment
Posted by Jennica
So, you’re going to bring your child in to get zapped! Congratulations. I always applaud treatment, because I know that some parents have struggled to get sufficient medical advice to understand that, no, this birthmark isn’t going away on its own, and will in fact only grow with the child. So treatment is an excellent step forward.
Let me walk you through a few points related to treatments, based on our own experiences. (Again, I’m a lay person, not a doctor, and this is anecdotal advice, but hey – that’s what the internet is for, right?)
1. Get it done under anesthesia.
There are doctors who treat port wine stains without general anesthesia. I think they’re crazy. Here’s why.
A few years ago, my son developed a little red-dot hematoma on his cheek. It, too, needed a laser treatment. Since it was so small, Dr. Z. (Addy’s dermatologist) told us to just come into his clinic, where he would do a quick zapping with a bit of topical anesthetic. That’s the normal practice for the fancy clients who want their unwanted capillaries zapped. It gave me a chance to see what’s usually done behind closed operating-room doors. So we went in, put on special sunglasses, and helped hold Clarence while the laser zapped him.
It was noisy! And powerful! Like lightning suddenly exploding: BZZZZ! BZZZZ! BZZZZ! Pause. Then again: BZZZZ! BZZZZ! BZZZZ! The impact to the skin is often described to us by adults as “being snapped by a rubber band over and over, a hundred times a second.” BZZZZ! I could see the impact on the skin.
We had to wait through a moment of silence, then: BZZZZ! Another moment of silence, then BZZZZ!
Clarence was a trooper, but he did cry a bit.
That was zapping just a tiny spot on his cheek. When we were all done, Dr. Z. looked at me and said, “Now you can see why we do port wine stains under anesthesia.” Yes, sir, INDEED, I can. The sheer acreage of a port wine stain demands it. These are not little varicose veins or spotty hematomas – they’re big and spacious, and need *gridwork*, not *spotwork*.
Why am I telling you this? So that you can feel confident in your provider’s choice to put your child under anesthesia. Some parents (and even some professionals, and definitely the coverage providers) feel uncomfortable putting children under anesthesia. They may quote a report that came out a few years ago vaguely linking multiple trips under anesthesia in a child’s first two years with later behavioral issues like ADD. But what usually isn’t addressed in those conversations is the fact that children who require multiple surgeries in their first two years of life might have complicated medical issues, and that it’s just as likely that the later behavioral issues are caused by the underlying medical condition, the effects of it, or simply growing up in a hospital, and not by any long-term effect of anesthesia. Port wine stain cases are unusual in that, in spite of the need for multiple surgeries, there usually isn’t a major underlying medical condition affecting development (except for Sturge-Weber Syndrome), so we really don’t have much to worry about.
Addy’s had forty-three trips under anesthesia, and she is (in my humble opinion), a well-adjusted genius.
I can’t recommend anesthesia heartily enough. Anesthesia takes what could be a difficult and stressful experience (“BZZZZ!”), and turns it into a glorified nap.
2. The Day Of Treatment
Let me repeat something from the last sentence above: from your child’s perspective, all she will experience is *a glorified nap*.
Parents, please remember that when you bring your child in for a laser treatment under anesthesia. There is no great terror here. You will be STRESSED BEYOND BELIEF. That’s okay, you’re her parent, you’re *supposed* to be stressed when your offspring is taken from you and given a gas to knock her out. Totally natural.
But when she comes in for an outpatient surgery, your child will experience something like this sequence of events, all of which are pretty harmless from her perspective:
- Arrive at hospital. (There’s a colorful mural on a wall. Pretty!)
- Check in; the nurse dotes on you by taking your height & weight and giving you hospital pajamas to change into. (What an AWESOME COLOR.)
- You wait for the various doctors and nurses to come and pre-check you. (Which gives you time to PLAY WITH TOYS. )
- Various doctors and nurses come to pre-check you. (Excellent opportunity to practice your pleases & thank-yous, and say your name & birthday a lot, while they smile at you. SO MUCH ATTENTION!)
- They wheel you back to the room. (A RIDE! AWESOME!)
- They put a mask on your face and help you sleep. (Zzzzzzzz)
- You wake up from your nap.
- You eat popsicles after your nap. BEST. DAY. EVER.
That’s pretty much it, from your child’s perspective.
Here’s the key: whether this is a positive or negative experience rests in your hands, parents. No matter how stressed you are, you must help your child see everything new in a positive light. You are the sky, she is the water, and she’ll reflect your attitude. Be sunny.
Think of a first ride on a rollercoaster – it could either be terrifying or exhilarating, and a child watches their parent’s reaction to help determine whether the New Thing is terrifying or exhilarating.
Help her enjoy her day by pointing out the pretty mural on the wall. Help her get excited about the hospital pajamas, no matter how ugly they are. Tell her to thank every nurse and tech and doctor who dotes on her, even if they’re just flatly doing their job. Point out how awesome it is that she gets to play with toys, even if she has the same ones at home. Act like the mask with the crazy gases is worth smiling about. When she wakes up, help her procure popsicles and be amazed together that she’s eating popsicles at that time of day, without even eating lunch, and make it sound like the best day ever.
Okay, so that’s her perspective. Now yours:
- You’re gonna cry. Accept that, make peace with it, stash a tissue in your pocket, and be ready. They’re knocking your baby out. The tears come, whether you want them or not.
- Your maternal instinct will DEMAND that you tackle the people wheeling away or putting a mask on your baby. “YOU TOUCH MY BABY, YOU DIE.” It comes up suddenly. It’s unexpected. And you were feeling so civilized today. To avoid getting arrested, suppress this instinct as much as you can. Good luck.
- Allow yourself to glance at the other families, patients, anyone else you see. Pretty much every single one is fighting a harder battle. This helps keep you grounded & sane.
Addy has enjoyed something about every surgery. She looks forward to each one. She wants to go back to see Dr. Z. and all the wonderful people at Children’s who dote on her and give her toys to play with and popsicles.
Next week, I’ll share a bit more insight on how we got her to like medical procedures, because a lot of intentional parenting went into it. But in the meantime, let me share a few other things to keep in mind that will help your whole week go better.
3. A few final medical tips
- In the days leading up to a surgery, play around with putting things in front of your mouth and your child’s, like an anesthesia mask. Make something out of a brown paper lunch bag if you have to – the point is to get her comfortable with something safe in front of her face. (Okay, here’s the obvious but necessary caveat: don’t use plastic bags or anything unsafe. Feel free to teach her the difference here.) Make it a trumpet; try breathing into it; play doctor. Play, play, play! Then, when an anesthesia mask is really put on her face, rather than freaking out (“Get that weird thing away from my face!”), she’ll recognize the game.
- Listen to the anesthesiologist when they tell you what they plan to do. There are many variations of the anesthesia cocktail they could give her (with or without anti-nausea, with or without steroid, with or without amnesia); take notes here so that you can, over time, determine what cocktail works best. (For Addy, it’s no steroids, no amnesia drugs, but with something for pain and sometimes a little something extra to help her sleep longer.)
- There’s an “anesthesia hangover” that lasts about 3-5 days. Your child might be weirdly more emotional than usual. More likely to break down and cry. Emotionally fragile. That’s just the anesthesia hangover, and it will pass. Warn her teachers, warn her caregivers, and warn yourself. She’s fine, just a little emotional. Give her grace.
- You probably won’t experience this, but there’s such a thing as “emergent delirium”; this affects mostly 3- and 4-year-olds, and occurs when a child ‘wakes up’ and appears functional, but their brain is still anesthetized. This happened to Addy at age 3; she seemed to wake up, but was still weirdly fogged. The ‘disconnect’ between awake & asleep brings on some unexpected behavior. (In our case, massive tantrums.) If you see your child completely breaking down post-anesthesia, don’t worry; she’s probably just processing the rest of the anesthesia, and IT WILL PASS SOON. Suddenly, the clouds part, and the child is normal again. The nurses can help you navigate this if it happens, but again, it’s unlikely.
These laser surgeries are nothing. No scalpel, no stitches, no chemo, no major complications. And yet they’re a big deal; you’re watching your child get knocked out for a medical issue, and your Maternal Instinct will be aroused. (DOWN, Mama Bear!) Allow yourself to maintain the perspective that this is a light burden, and that it comes with the blessed opportunity to help our children navigate the modern world with lovely marks on their faces, and to endow them with depth of character early in their young lives.
But just, like, try not to punch the nurse. Okay? Okay.
Port Wine Stains, Hemangiomas, and (some) Complications
Posted by Jennica
Parents, if your darling new baby has a red birthmark, you will want to know the difference between a port wine stain and a hemangioma, two common types of vascular birthmarks, and what some of the related complications might be.
I can tell you what I know – which, admittedly, isn’t much, and is, I’m afraid, heavily anecdotal. But, no matter; I’ll still share it.
Port Wine Stain vs. Hemangioma
A port wine stain, which is what Addy has, is usually flat at birth, but then it grows over time. That growth means that a port wine stain will often become raised & nodular, especially if left untreated.
A port wine stain is a proliferation of blood vessels associated with a particular nerve. That nerve, otherwise responsible for telling its partner blood vessels in utero to “Stop growing!”, missed giving that critical signal at some point during development – so the blood vessels kept growing and growing. (In Addy’s case, the error is associated with the middle branch of the trigeminal nerve, on the right side of the face.) As a result, the capillaries are abnormally wide in diameter (like, over 40x wider).
A hemangioma, on the other hand, is raised at birth – you can feel it if you run your finger over the skin – and it may grow a bit in the first year, but then it will recede or ‘implode’ on its own.
A hemangioma is a cluster of blood vessels by the surface of the skin, sometimes medically referred to as a benign ‘tumor’ of blood vessels. It’s often very bright red. These are the common “strawberry marks” we all know on babies. They usually fade on their own.
I can’t tell you how many birthmark misdiagnoses I’ve heard. Many of them were directed to us by well-wishers, including nurses who told us “Oh, that’s just a hemangioma, it’ll go away!”; others have been directed to some of my readers by aloof primary-care doctors who weren’t familiar with port wine stains. Get your child to a specialist who understands vascular malformations (a good dermatologist should know the difference), and get the right diagnosis.
Here’s why: if your child has a hemangioma, it will probably disappear on its own, and if it doesn’t, well, you can cross that bridge when you get there. But they usually go away without intervention.
If your child has a port wine stain, though, it will not go away on its own; in fact, it will grow with your child. And as your child develops, their blood vessels and the skin above them will only develop & toughen, making it harder to eliminate the stain later. The worst medical advice in that critical first year is “Ehhh, let’s just see if it goes away on its own.” It won’t. It will only toughen. We were lucky – Addy went in for her first surgery at 5 weeks old, and had 9 more before her first birthday.
Complications
Complications can arise depending on how ‘deep’ the birthmark is, and where it’s located, which are determined by when the error occurred in utero.
If the error of a port wine stain occurred earlier (i.e., the nerve missed giving that critical signal to “Stop Growing!” to its associated blood vessels), then the port wine stain will be deeper in the skin, and wider on the body. For example: Addy’s stain covers much of the right side of her face (along the V2 branch of the trigeminal nerve), and is relatively difficult to treat, hence the 43 surgeries so far. It’s deep.
Meanwhile, her friend has a small stain along the exact same V2 branch of the trigeminal nerve, but it’s the size of a half-dollar coin on her cheek, and it disappeared after a half-dozen laser treatments. That’s because the friend’s error occurred later in utero, while Addy’s occurred earlier.
Other kids have massive vascular malformations that erred even earlier than Addy’s; one young woman told me that her brother was born with a large one that totally covered one shoulder and down onto his back, and it was so large (and deep, and thick) at birth that the doctors weren’t sure if he would be okay. He avoided contact sports, but otherwise has been living a healthy life.
Depending on where the stain is, a port wine stain can cause other complications. For example, if the stain is on the V1 branch of the trigeminal nerve (the optical branch, along the forehead), the risk is significantly higher for Sturge-Weber syndrome, which is a constellation of issues stemming from having malformed blood vessels in the head, including calcifications in the brain (which can hinder brain development) and seizures. An MRI helps diagnose Sturge-Weber issues in the brain.
Since Addy’s port wine stain touches onto her forehead, she had an MRI at 5 months of age, to make sure that there were no vascular malformations in her brain; all was clear.
But glaucoma is definitely a concern, since the proliferation of blood vessels can also cause undue pressure on her eye. She is checked for glaucoma annually.
Of course, glaucoma isn’t the only eye issue; as you’ve read here, Addy’s tear drain was pinched off by the pressure of all the encroaching blood vessels around it. She had a tube put in a few years ago to try to prop it open. Even though it fell out shortly afterward, it did successfully open up the plumbing for a while, and it bought her some development time. Unfortunately, she’s been tearing up again in her right eye, so we may have to do it again.
The port wine stain is also in her mouth. This is fascinating! As the right and left sides of the head develop in utero, they ‘meet’ in the middle; thus, any error tends to only show up on one side of the face. Addy’s face is split down the middle, even down to her tongue and uvula! If you ask her to open up her mouth, you’ll see her tongue is half red, half pink – and if you look farther back, even her uvula is precisely half red, half pink.
The extra bloodflow to the right side of her mouth meant that her teeth developed earlier, and popped out of her gums earlier. (And, luckily, they popped out fast. Teething wasn’t so bad!) As a baby, she had an adorably lopsided smile for a short time until her left side came in.
But now, all that extra bloodflow and tooth development means a lot of crowding; the well-populated, well-nourished right side of her mouth is crowding out the left, and an extra tooth is popping in above the others (affectionately called ‘The Snaggletooth’), because it doesn’t have any place to go. So, we can add significant orthodontia to our 2019 budget.
When she brushes her teeth, bleeding from the right side isn’t uncommon. In the wintertime, she gets one-nostril nosebleeds on the right side. We try to minimize all possible injury to her face, gums, nose, and scalp on the right side, because she bleeds more than the average bear in those places. And, if you look closely, you’ll see that her bones are actually a bit bigger on the right side of her face, due to the extra bloodflow. It’s not actually a problem (or even noticeable) for Addy, but I know another little girl with a port wine stain who had to see a craniofacial surgeon to see if anything could be done about some too-fast bone growth along her stain.
So, there are complications to these port wine stains. Hemangiomas probably bring various complications, too, especially very large ones, but my experience is limited to port wine stains on the face. These are simply some of the things we’ve watched & worried over with Addy. Each birthmark is unique, so please don’t hesitate to contact me with questions and pictures if you want a mom’s advice. I’m not a doctor, and I will tell you to ‘get thee to a dermatologist’ if you haven’t yet, but I’m happy to navigate these waters with you.
For the sake of trivial interest in birthmarks, I can tell you that there’s another type of birthmark called a nevus, which is a proliferation of skin pigmentation, rather than blood vessels. (Have you ever seen someone with a really dark brown or black birthmark? Sometimes hairy? That’s a nevus.) We know a little girl with a nevus on her forehead, and the complication her parents have to worry about is skin cancer. Their pre-emptive treatment is skin grafting. (I’ll take lasers any day!)
Also, among blood-red marks, there’s even a third type after Port Wine Stain and Hemangioma: Hematoma. In short, a hematoma is a red spot that looks like a hemangioma, but it usually comes about by injury or disease. Clarence ended up with a small hematoma on his face after an injury, and he got to have a laser session with Dr. Z., but I’ll tell you more about that in another post.
So, there: you’re ready to win obscure trivia questions about birthmarks! You’re welcome.

It’s not always easy to see, but check out the way her teeth are pushed over from the port wine stain on her right to the left — lots of activity on the right side! Lots of extra blood flow for growth.

Addy graciously let me photograph the inside of her mouth; the port wine stain invades her mouth, but only on the right side.
The Stranger in Macy’s
Posted by Jennica
It’s good to be back! For the last year, I’ve been writing more for my mother than my daughter over at CaringBridge (FYI — she’s doing great!).
But Addy’s EBC speech (below) brought me back here, and I’ve been wanting to share a sweet story with you from a recent outing.
Keith and I were walking with the kids through a Macy’s department store one afternoon. We move slowly as a herd, and passing all the shiny things in the jewelry department slowed us down even more. With plenty of time to glance around at the other patrons, I saw a woman standing with her husband at the jewelry counter. As she turned her head back and forth in conversation between her husband and the employee helping them, I noticed a big, dark, red splotch on the front of her face.
I stared, like any good 5-year-old would do, but tried to be at least a little bit discreet while I determined if it was a birthmark or a burn scar or something else. With each mark being so personalized & unique, it can be hard to identify from a distance; you just know there’s something big there.
She didn’t notice me staring, thank goodness, but I quickly realized that it was because she had locked in on Addy. She was staring at Addy.
I nudged Addy to get her attention from the shiny things for a second, turned her toward me, and whispered excitedly, “Don’t turn and stare, but I’m pretty sure there’s a lady over there with the exact same stain you have.”
Whenever we encounter someone else with a unique feature, like the darkness of a birthmark, the baldness of alopecia, the stature of dwarfism, or the gap of a missing limb, I treat it like a celebrity sighting. It’s all in the attitude – a combo of “Ohmygoodness they have something super-unique too! Agh!” and “Be cool, be cool.” With that, my children have learned that people who ‘stick out’ (like celebrities, or Addy) are totally positively awesome, and that they might (like a celebrity) not want to be disturbed. With small children, one can never teach too much discretion.
So when I told Addy there was another person just like her nearby, her eyes got big and excited and she got twitchy as she itched to turn and look but knew better. She stage-whispered, “Where?” “Behind you.” Addy turned naturally as if to look at more jewelry, glanced at the woman discreetly, then played it cool, turning to me, “It’s even on the same side!”
I got the impression that the same thing was happening between the couple buying jewelry. I thought about introducing ourselves, but hesitated; this woman was a bit older than I was, which means she had grown up before the unique-is-awesome attitude pervaded the culture as widely as it has by now. People from Generation X and earlier don’t always have good memories of growing up with their unique feature; some came from families that never spoke of the birthmark at all. They’ve made reluctant peace with it, but they’re sick of being noticed in public; in their experience, being noticed isn’t a good thing.
There wasn’t much time to think about it, though, because the next thing I knew, the woman was leaving her bag with her husband and walking toward us. I turned expectantly, as if we were going to engage in the usual polite grown-up introductions, but she walked right by me and, without saying a word, engulfed my daughter in a bear hug.
Addy hugged her right back. They stayed there for a long, long moment, and I heard this stranger speak quietly into Addy’s hair: “You are so beautiful. You are so beautiful. Don’t ever let anyone tell you otherwise. You are so beautiful.”
And that’s how we met. After detangling from Addy, the woman said to us, “I’m so excited! I mean, I often see other birthmarks, but it’s really rare to see someone with a stain, just like mine, on the right side!” We talked about how pretty it is, the way it ‘sweeps’ up to the hairline. Addy told her proudly that she’s had forty-something surgeries, and the woman nodded: “I had thirty-seven.” I just about fell over – this woman’s stain was really dark! These two birthmarks were similar even in their resistance to treatment. “Keep zapping!” she encouraged. Addy told her about having a tube down her eye, and getting checked for glaucoma, and the woman nodded, “Yep! Me too.”
I’m so grateful that this woman came over. I’m grateful for her confidence. I’m grateful for her willingness to bear-hug a stranger’s kid. My daughter got to meet someone like her, someone she could identify with, someone who’s walked in her shoes first.
Addy talked about it afterward like she’d been personally approached by a celebrity.
And, in a way, she had.

























